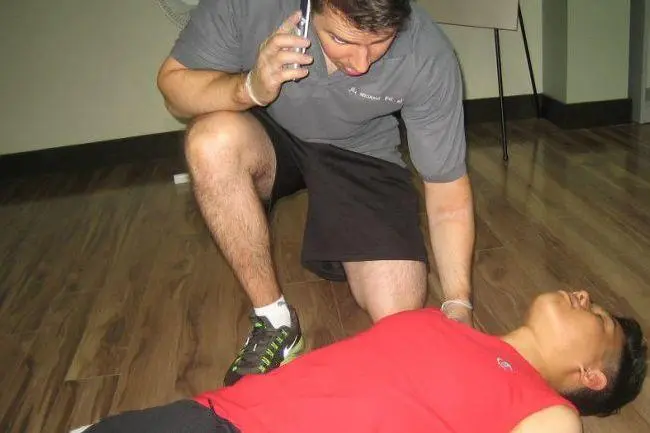
The most popular combined first aid and CPR course in Kelowna is standard first aid. This course includes training in CPR level “A”, “C” or “HCP”. AED training is included. Certification is valid throughout Canada for 3 years.
This course is one of the most popular one day workplace approved programs available. Commonly referred to as “basic first aid and CPR”, this course teaches basic rescue techniques for participants. AED training is included in this course that provide certification that is valid for 3 years.
Individuals that work in the childcare / daycare industry in Kelowna are required to be certified with emergency childcare fist aid. This one day course includes training in CPR level “B” and in the use of automated external defibrillators (AED).
At Kelowna First Aid we proudly offer 3M mask fit testing. This 15 minute test is designed for individuals requiring qualitative mask fit testing for the workplace, school or lab. Individuals enrolled in this short course will learn about testing masks, ensuring they work as well details behind the masks used. We currently offer N95 testing multiple times throughout the week. For more information visit our respiratory mask fit testing page.
3M Masks
Do you need 3M masks in the workplace, home or school? Visit our mask sales page to view the various masks that we have for sale that meet CE and FDA standards. We are a authorized sales provider of these masks and we can provide almost any quantity of masks. Free shipping and handling throughout Canada. Click here for more information about our masks or to purchase.
Welcome To St Mark James Training - Kelowna First Aid
Do you need to speak someone about registering for a course in Kelowna First Aid? Give us a call at 1-250-277-1944 or request a call back from us by clicking the following button
We offer the lowest prices on all of our courses. Check out a full list of all of our courses as well as our prices by clicking the following button
We offer on-line registration. View a full list of all of our upcoming courses by clicking the following button
Book a private course for a group of any size. We can teach a recertification, food safe, safety and workplace approved first aid and / or CPR programs at your training facility or ours. Use our contact us page to book a course with us.
Kelowna First Aid Courses

Standard First Aid
Kelowna First Aid proudly offers workplace approved standard first aid courses. Standard first aid, also referred to as intermediate first aid, is one of the most comprehensive courses that we have to offer. Individuals and students from a variety of backgrounds are required to be certified in this course.
Emergency First Aid
We proudly offer emergency first aid training in Kelowna, B.C. This course, also referred to as basic first aid, is designed to introduce rescuers to managing and recognizing basic emergencies. Individuals participating in this CPR and first aid class will also be taught fundamental CPR skills.
Emergency Childcare First Aid
We proudly offer one-day emergency childcare first aid, CPR and AED training at our Kelowna training center. This course is designed for individuals that need one day first aid, CPR and AED training and work.
CPR Courses

CPR level A
Kelowna First Aid offers a number of different CPR levels. The most basic CPR course offered is CPR level “A”. This course takes approximately 4 hours to complete and teaches candidates basic CPR skills for rescuing adult victims.

CPR level C
We proudly offer one of the most popular and comprehensive CPR level’s for lay rescuers. CPR level “C” teaches candidates CPR techniques for victims of all ages (adults, infants and children). Participants will also learn to do CPR with patients.
CPR HCP
We proudly offer this popular workplace and academic approved CPR “only” program. CPR level “C” for health care providers (also known as CPR “HCP”) is the most comprehensive stand-alone CPR course that is offered. This course teaches candidates CPR techniques.
CPR Courses
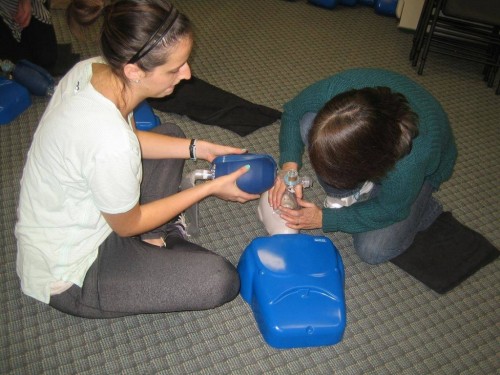
Emergency First Aid Recertification
This workplace approved course is specifically designed for candidates that want to renew previously acquired and current emergency / basic first aid awards. CPR recertification is included in this course and candidates can opt for either CPR “A” or “C” renewal with the class.

Standard First Aid Recertification
We proudly feature renewal courses for candidates that need to re-certify expiring standard / intermediate first aid certificates. This course is specifically designed for candidates that have previously completed a credible standard / intermediate first aid course, been awarded the certificate and need to renew the award.
Here is a List of Our Next 60 Courses:
| Event | Venue | Spaces Remaining | Date | |
|---|---|---|---|---|
| Private BLS- Orchard Park Dental | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
1 |
|
Register |
| Standard Childcare First Aid Course in Kelowna | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
8 |
|
Register |
| Standard First Aid Course in Kelowna | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
5 |
|
Register |
| First Aid and CPR Re-Certification in Kelowna | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
3 |
|
Register |
| Qualitative Respiratory Mask Fit Test | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
6 |
|
Register |
| Standard Childcare First Aid Course in Kelowna | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
unlimited |
|
Sold Out |
| Standard First Aid Course in Kelowna | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
unlimited |
|
Sold Out |
| Basic Life Support (BLS) / CPR and AED Course in Kelowna | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
unlimited |
|
Sold Out |
| Basic Life Support (BLS) / CPR HCP & AED Re-Certification in Kelowna | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
unlimited |
|
Sold Out |
| Emergency Childcare First Aid Course in Kelowna | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
unlimited |
|
Sold Out |
| Emergency First Aid with Basic Life Support (BLS) Course in Kelowna | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
unlimited |
|
Sold Out |
| First Aid and CPR Re-Certification in Kelowna | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
unlimited |
|
Sold Out |
| Qualitative Respiratory Mask Fit Test | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
unlimited |
|
Sold Out |
| Standard Childcare First Aid Course in Kelowna | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
8 |
|
Register |
| Standard First Aid Course in Kelowna | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
6 |
|
Register |
| Basic Life Support (BLS) / CPR and AED Course in Kelowna | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
4 |
|
Register |
| Emergency Childcare First Aid Course in Kelowna | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
5 |
|
Register |
| Emergency First Aid with Basic Life Support (BLS) Course in Kelowna | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
5 |
|
Register |
| First Aid and CPR Re-Certification in Kelowna | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
1 |
|
Register |
| Qualitative Respiratory Mask Fit Test | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
8 |
|
Register |
| Emergency Childcare First Aid Course in Kelowna | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
unlimited |
|
Sold Out |
| Emergency First Aid with Basic Life Support (BLS) Course in Kelowna | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
unlimited |
|
Sold Out |
| Basic Life Support (BLS) / CPR and AED Course in Kelowna | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
unlimited |
|
Sold Out |
| Basic Life Support (BLS) / CPR HCP & AED Re-Certification in Kelowna | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
unlimited |
|
Sold Out |
| Standard Childcare First Aid Course in Kelowna | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
8 |
|
Register |
| Standard First Aid Course in Kelowna | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
6 |
|
Register |
| Basic Life Support (BLS) / CPR and AED Course in Kelowna | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
2 |
|
Register |
| Basic Life Support (BLS) / CPR HCP & AED Re-Certification in Kelowna | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
2 |
|
Register |
| Emergency Childcare First Aid Course in Kelowna | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
1 |
|
Register |
| Emergency First Aid with Basic Life Support (BLS) Course in Kelowna | Unit #205 1634 Harvey Ave, BC V1Y 6G2 Kelowna British Columbia Canada V1Y 6G2 |
3 |
|
Register |
What Our Students Say About Us!

 Joshua AdrianBrynn was an amazing instructor. Very knowledgeable and easy to understand which made the course pleasant and enjoyable. If you're looking for certification in the kelowna area....this is the place to go! Thank you!
Joshua AdrianBrynn was an amazing instructor. Very knowledgeable and easy to understand which made the course pleasant and enjoyable. If you're looking for certification in the kelowna area....this is the place to go! Thank you! Laura ParisisHans was very educational and helped make this class fun while making sure we learned everything we needed!
Laura ParisisHans was very educational and helped make this class fun while making sure we learned everything we needed! Nim SidhuHans was a great instructor. He brought humour into a class that could be very dry and made it an enjoyable time. His experience in the field is evident and he is extremely knowledgeable. Thank you! I will be back to renew it!
Nim SidhuHans was a great instructor. He brought humour into a class that could be very dry and made it an enjoyable time. His experience in the field is evident and he is extremely knowledgeable. Thank you! I will be back to renew it! Kristina TayHans was a great instructor and made the class interesting! Thank you for the great class!
Kristina TayHans was a great instructor and made the class interesting! Thank you for the great class! Adventure Seeker1306Completed my SFA here today with instructor Brynn. Brynn really gets the point across in a different way and approaches it from another angle. He is very knowledgeable and brings a toolkit of lived experiences. I quite enjoyed it!!! Thank you Brynn!!! 😁😁
Adventure Seeker1306Completed my SFA here today with instructor Brynn. Brynn really gets the point across in a different way and approaches it from another angle. He is very knowledgeable and brings a toolkit of lived experiences. I quite enjoyed it!!! Thank you Brynn!!! 😁😁 Jasmine PannuVery professional the teacher was well educated in health care. I found his jokes hilarious. He is easy to understand and explains things in simple terms. As a healthcare worker his techniques for cpr are memorable. Please have more teachers like this. He made the class as lively as possible and answered each question in depth regardless how arrogant some questions were. I highly recommend this class. Thank you.
Jasmine PannuVery professional the teacher was well educated in health care. I found his jokes hilarious. He is easy to understand and explains things in simple terms. As a healthcare worker his techniques for cpr are memorable. Please have more teachers like this. He made the class as lively as possible and answered each question in depth regardless how arrogant some questions were. I highly recommend this class. Thank you. Tyler OlsonFacts first aid is amazing, I did my OFA level 3 first aid training with Greg and Katie, and it was great, both instructors are very knowledgeable, smart, super friendly, and want to help you learn the skills you need, they both enjoy doing what they do, and it's a very positive learning center
Tyler OlsonFacts first aid is amazing, I did my OFA level 3 first aid training with Greg and Katie, and it was great, both instructors are very knowledgeable, smart, super friendly, and want to help you learn the skills you need, they both enjoy doing what they do, and it's a very positive learning center
Serving Kelowna and interior British Columbia with the lowest priced, least canceled and highest quality first aid courses, food safe and CPR training since 2014 with a commitment to make the community safer.